Most home care agencies assume their biggest revenue problems come from outside forces like low reimbursement rates, staffing shortages, or slow billing cycles.
But in reality, a significant amount of revenue is lost much earlier, and much more quietly.
It happens in the gap between what’s authorized and what’s actually scheduled.
This isn’t a dramatic, obvious issue. It doesn’t show up as a single error or a missed claim. Instead, it happens gradually, week after week, across patients, services, and coordinators, until the impact becomes impossible to ignore.
The Illusion of “Approved Care”
Authorizations give agencies a sense of security. Once services are approved, it feels like the hard part is done.
You can clearly see everything on paper: the payer, the services, the billing codes, the approved weekly hours, and the total hours available within a date range. A patient might be authorized for 23 hours per week under PCA, another for 2 hours under HMK, each tied to specific billing codes and insurance plans.
On the surface, it looks organized and under control.
But authorizations only define what can happen. They don’t reflect what is happening.
And that’s where the disconnect begins.
Where the Revenue Actually Slips
If a patient is approved for 24 hours of care per week but only 8 hours are scheduled, nothing immediately breaks. There’s no alert, no urgent notification. Care is still being delivered. The system still looks active.
But 16 hours of approved, billable care simply never happen.
Now multiply that across dozens of patients.
That’s not a small inefficiency—it’s a structural revenue leak.
At the same time, the opposite problem often exists in parallel. Services can be scheduled beyond what was authorized, especially when teams are juggling multiple cases and changing needs. Those extra hours may get delivered, but they don’t always get paid. Instead, they turn into denied claims, rework, and compliance exposure.
So agencies end up losing revenue from both sides—underutilization on one end, and overextension on the other.
Why Most Agencies Don’t See It
The issue isn’t that agencies don’t care. It’s that the visibility isn’t there.
Authorizations live in one place, detailed and structured. Scheduling lives somewhere else, constantly changing. Without a clear connection between the two, teams are left making decisions based on partial information.
A scheduler might fill shifts based on availability, not realizing a patient still has unused authorized hours. A coordinator might focus on urgent cases, without seeing where the largest gaps in utilization actually are.
Over time, this creates a kind of operational blindness. Everything is technically being tracked—but not in a way that reveals what’s missing.
What Changes When You Connect the Two
When authorized hours and scheduled hours are placed side by side, the picture becomes very different.
Instead of assumptions, you get clarity.
You can immediately see when a patient is significantly below their authorized time—like a case where only 8 hours are scheduled against 24 approved. That’s no longer just a number; it’s a clear opportunity to recover revenue and improve care delivery at the same time.
You can also spot when a service is drifting into overscheduled territory, before it turns into a billing issue. What would have been caught weeks later is now visible in real time.
This isn’t about running more reports. It’s about seeing the right information in the moment decisions are being made.
How INMYTEAM Approaches This
At INMYTEAM, we built this visibility directly into the workflow.
The Authorizations dashboard gives agencies a clean, centralized view of everything that’s been approved—patients, services, billing codes, payers, weekly hours, and total authorized hours. It’s structured, filterable, and easy to navigate, so teams always know what care is allowed.
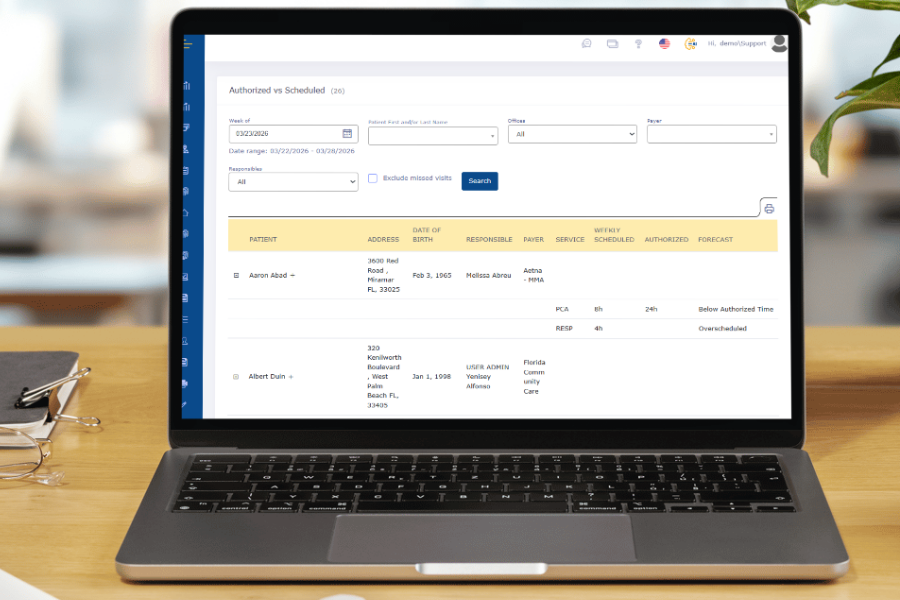
But the real shift happens in the Authorized vs Scheduled view.
This is where the data becomes actionable. For each patient, you can see what’s scheduled for the week, what’s authorized, and whether those two are aligned. When they’re not, the system makes it obvious—highlighting cases that are below authorized time or already overscheduled.
Instead of digging through multiple screens or spreadsheets, your team can immediately identify where attention is needed and act on it.